Using user-centered design to address neonatal hypothermia in low resource settings
2022.9.14
There is a strong need to adapt existing products or processes to humanitarian settings or develop new solutions. Médecins Sans Frontières (MSF) Japan office also has been contributing to these challenges, often in partnership with external partners. For example, since 2019 MSF Japan has been working with Design that Matters (DtM), an American NGO, to develop a solution to prevent hypothermia in newborn babies.
“What happens when a high-tech product is made based on invention or engineering genius but it doesn’t work? The excuse ‘they used it the wrong way’ is not acceptable,” says Tim Prestero, CEO of Design that Matters (DtM). Due to a lack of spare parts, engineers, stable power supply, different climates, etc., high-tech medical devices used in developing countries are often unused or broken and discarded after only five years.
Design that Matters develops medical devices for low-resource settings with a number of business partners and volunteers. A recent successful innovation is a phototherapy device for treating jaundice in newborns. The device is now in use in 33 countries across Asia, Africa and the Caribbean.
Prestero’s frustration with badly designed products pushed him to switch from engineering to design: “There are no ‘dumb users,’ only dumb products”.

Founder and CEO of Design that Matters
To develop solutions that fit the needs of our patients and field staff, user-centered or patient-centered design is at the heart of MSF Japan’s Innovation projects. Such a process puts users and patients central. This allows us to develop a product that is durable, easy to maintain, simple to use and “actually useful,” says Prestero.
Applying user-centered design to hypothermia

May 2022 © MSF
MSF Japan has been working with DtM to develop a solution to neonatal hypothermia in low resource settings. A baby’s ability to regulate its own body heat is weak. They are easily affected by room temperature changes, leading to hypothermia. In developed countries, newborns are put directly under a radiant warmer (treatment) or incubator (prevention) for thermal management. Neonatal hypothermia in developing countries is often overlooked. According to a statistics, about 40% of newborn mortality in low resource settings is correlated with the incidence of hypothermia(*).
High-tech products to prevent and treat hypothermia are often not available, practicable or usable in facilities of the developing world. “So the challenge is adapting practices of newborn thermal management of a European, US or Japanese setting to a low resource setting,” says Prestero.
MSF Japan does not have the expertise in-house to develop and build a solution. As a result, we partnered with DtM in 2018. In turn for DtM, partnering with MSF provides access to medical activities in low resource settings. Adaptation requires knowing the local environment and contexts, but “the areas with the greatest need are often the hardest to reach. We can’t go there on our own”. MSF has medical operations in many parts of the world where people are most in need. Prestero says: “We may know a lot about design, but we are not pediatricians, not an aid organization. By partnering with MSF, we get access to the expertise for how care is provided, and then we can figure out how to adapt the device to meet MSF’s needs.”
- *Hypothermia is recognized as a comorbidity factor to the three main direct causes of neonatal death: preterm birth, severe infection, and asphyxia [1]. Preterm birth is responsible for 60% to 80% of all newborn deaths, and preterm babies are at a higher risk for developing hypothermia. Preterm babies require immediate and continuous warming in order to survive.
- [1] K. Lunze, D. E. Bloom, D. T. Jamison, and D. H. Hamer, “The global burden of neonatal hypothermia: systematic review of a major challenge for newborn survival,” BMC Med, vol. 11, no. 1, p. 24, Dec. 2013, doi: 10.1186/1741-7015-11-24.
Assessing contexts and needs
The project started with a patient journey mapping and interviews with nearly 50 staff from MSF, health facilities and industry players. These data were used to analyze the needs and potential gaps. Prestero: “In fact, most problems are process or training problems. With warming, however, we discovered gaps that cannot be addressed by training and protocol alone. Babies can still become hypothermic, for example, in the short distance to transport from labour and delivery to the newborn unit.”
Four characteristics emerged as essential for a baby-warmer: portable, easy to use, easy to clean and inexpensive”. In addition, to keep to user-centered principles for low resource settings “it must also be durable and require minimal training in use and maintenance”, says Prestero.
A market study was implemented to see if any current available devices could fill this gap and fit with current MSF policies. The study found that no existing devices fulfill these criteria. “What we are really trying to design is solution to these gaps. The outcome is reducing hypothermia. This means that the product has to fit into the whole system of procurement, training, maintenance and cleaning.”
Building on insights from this first phase, a prototype that meets all the requirements was developed. The prototype was built by design engineer Saige Sunier (24) who joined DtM after graduating from university with a degree in biomedical engineering. “I used CAD software to design and repeated 3D printing processes. None of the technology used is complicated and the prototype was made in two months", explains Sunier. Prestero adds, “Twenty years ago, medical device development would have taken a team of more than ten people, hundreds of thousands of dollars of equipment and a long period of time. But this prototype was built by herself in our workshop.”

On-site prototype test

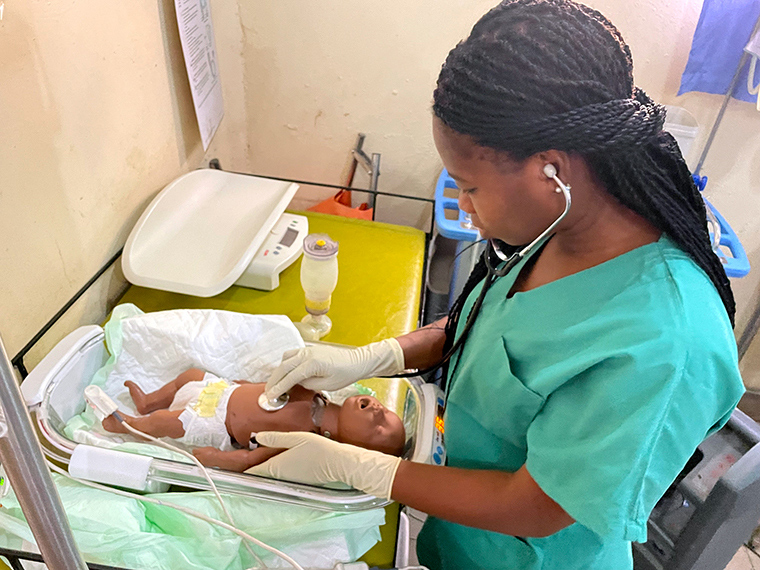
In May 2022, DtM and MSF Japan staff travelled to Kano in northern Nigeria, Nigeria’s second largest city, to gather feedback from local staff in an African context. The MSF facility in Kano assists with an average of 200 births per month. There is also a large state-run referral hospital in the city, where about 1,000 babies are born every month.
First, staff at both facilities were asked to list the characteristics they consider essential for the device and the procedures for any medical activity.


Staff were also shown the baby warmer prototype. More than 25 medical and non-medical staff held the device in their hands. Response from the staff was positive—with some even requesting the device be equipped in all maternity projects of MSF.
Also unexpected needs for the device were revealed. In urban Kano, referral transport takes 45 minutes, but in rural areas it may take more than five hours. Most Africa’s roads are unpaved and bumpy, and the ambulance can shake heavily. “We need to ensure safety during transport. We also need to increase battery life,” says Prestero. The team gained insights on use requirements that might not have been discovered, had they not visited the sites.
MSF Japan and DtM will continue to improve the prototype. Additional visits to the field are planned to test next design versions. The vision is to deliver a cheap, marketable product that will set a new standard for the treatment of neonatal hypothermia in low-resource settings in the next 18 months.
Open to collaboration opportunities with external partners, MSF aims to continue finding the solutions to challenges in the fields—in order to improve our patients’ lives.
